Case Study
Netherlands – Value Based HIV Care
-
Context
OLVG hospital is the largest HIV clinic in the Netherlands, taking care of over 3,500 people living with HIV. It is the mission of the OLVG HIV care team to provide care beyond 90-90-90 with a strong focus on health related quality of life (the local cascade of care figures are 89-98-97%).
-
Introduction
In order to measure the quality and costs of our care in a transparent way, we applied the value based healthcare principles to our HIV care; “Value Based HIV Care (VBHiC)”.
-
Aims
The aim of Value Based HIV Care is to improve the health outcomes of our patients, including their health related quality of life, with the patient being in optimal control over his or her health.
-
Method
In close collaboration with our patients, we defined HIV care outcome indicators: therapy effectiveness, therapy tolerance, retention in care, mortality, cardiovascular risk and quality of life. A VBHiC HIV app “Happi” was launched, showing these indicators at a dashboard on the smartphone and containing other features as well, such as a travel algorithm, appointment reminders, and newsletters from patient organisations etc. (www.happiapp.eu)
-
Results
Defining health goals (outcome indicators) together with patients, helps both patients and caregivers understand what points to focus on for improvement at consultation or between OPD visits. Effects of interventions in the care process on both the quality of care and the costs are visible over time. For example, showing cardiovascular risk as a structured part of the consultation leads to more smoking cessation and thus reduction in cardiovascular risk. Addressing anxiety, depression, lack of social support and/or experienced stigma helps improve quality of life which will subsequently lead to less health care consumption. Our “no show” protocol has led to a decrease from 20% no shows to less than 10% and a lost follow up rate of < 1%. The freely available “Happi App” helps the patient take more control over his or her health. In an innovative so-called “bundle payment contract” with a large health insurer we have managed to improve quality of HIV care while subsequently reducing costs.
-
Recommendations
Value Based HIV Care provided us with clear indicators of quality of care and related costs. Better interventions can be developed to further improve the health outcomes of our patients. Quality of life for example can be further improved by addressing quality of life domains like anxiety, depression and stigma structurally. Furthermore, the best interventions for experienced stigma still have to be established.
-
Definitive Outcome Indicators
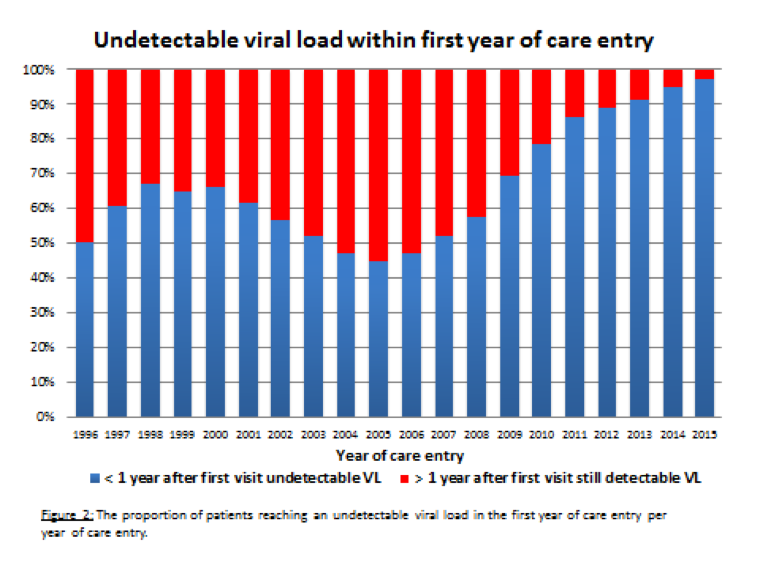
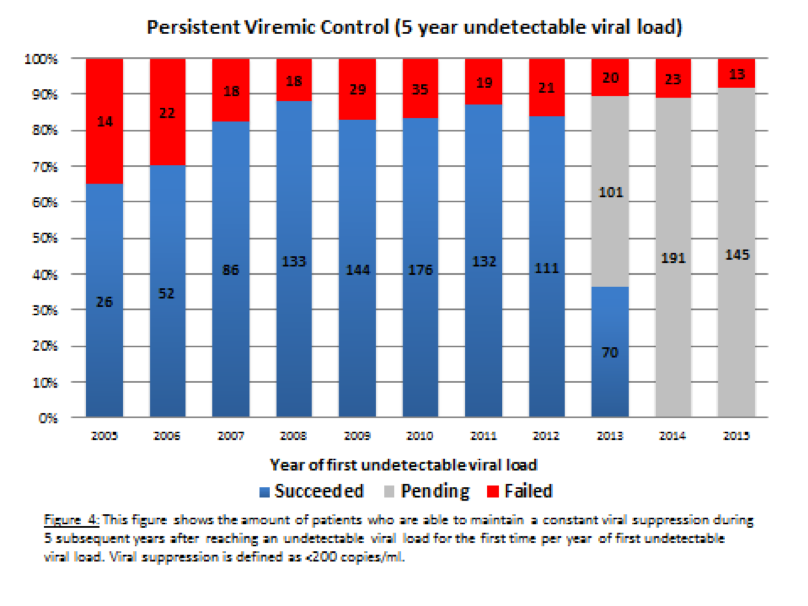
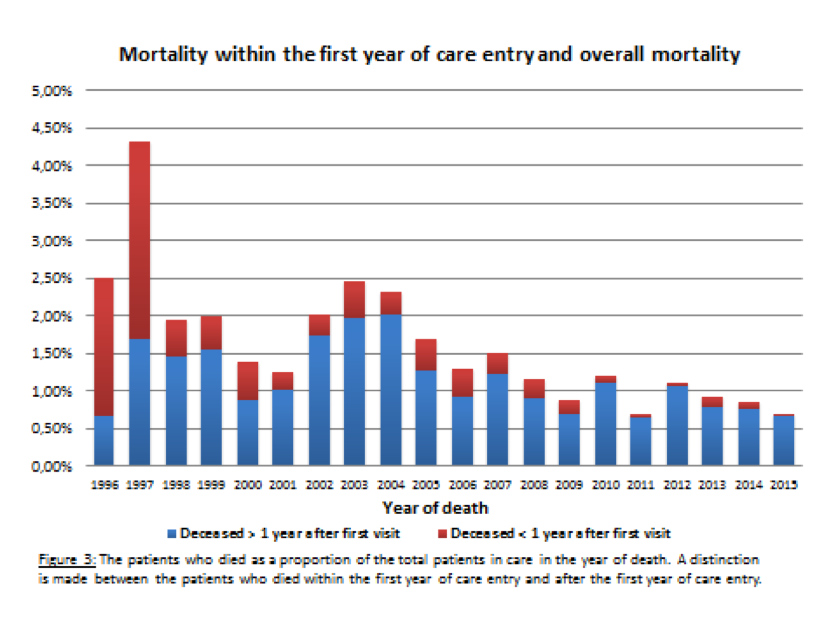
Tier Outcome indicator Definition 1 1: Undetectable HIV load within the first year of care entry The proportion of patients reaching an undetectable viral load in the first year of care entry per year of care entry 1 2: Quality of life within the first year of care entry Scores on questionnaires* covering seven different domains: quality of life, anxiety/depression, stigma, social support, sexuality, self-esteem and sleeping difficulties 1 3: Mortality within the first year of care entry Number of deceased HIV patients within one year after first visit with documentation of the cause of death 2 4: Retention in care The percentage of patients with at least one HIV load measurement or visit within 365 days 2 5: Therapy effectiveness (persistent viremic control) Continuous viremic control (HIV load below 200 copies/ml during 5 years after first time below the detection limit 2 6: Therapy tolerance Percentage of patients without intolerance (=cART switch due to adverse reactions or intolerance score >5). 2 7: Cardiovascular risk The cardiovascular risk in the overall HIV population using the SCORE-NL calculator (www.scoremeter.nl); sub indicator incidence of cardiovascular events 3 8: Quality of life every subsequent year Same definition as in indicator 2 but then for every subsequent year 3 9: Overall yearly mortality Yearly number of people deceased in the overall population with documentation of cause of death *QoL domains: Quality of life (SF-12), anxiety/depression (Hospital Anxiety Depression Scale; HADS), stigma (short stigma scale), social support (SSL12-I), sexuality (Incentive motivation model and Natsal-SF), self-esteem (SISE), sleeping difficulties (SCL90-Sleep) and perceived side effects.
-
Happi App
Mission
The mission of the Happi App foundation is to minimize the impact of being HIV infected on the patient’s daily life.
Features
- Happi App applies the value based healthcare principle by translating laboratory parameters and answers to quality of life questionnaires into health goals (=outcome parameters) and showing them in a dashboard on a mobile phone
- Happi App has the ability to be a personal health record; a safe connection has been realized between the app and the electronic patient record at OLVG hospital with more hospitals to follow.
- Happi App is frequently used in the Netherlands (also without a hospital connection) and can be used worldwide (available in English)
- The app contains other features like a travel algorithm, a pill – and appointment – reminder, a periodic newsletter from the Dutch patient organization, an automatic cardiovascular risk calculator and the ability to fill in quality of life questionnaires.
User statistics
Within 9 months, more than 10% of PLHIV in the Netherlands have downloaded the app and are using it.
Stakeholders support
- The Dutch HIV patient organization HVN is actively promoting Happi App on their website and offering periodic newsletter through the app
- A large health insurer (Zilveren Kruis) has strongly supported the development of Happi App as part of the value based HIV care cooperation with OLVG hospital
- Both the Dutch organization of HIV physicians (NVHB) and the HIV nursing organization (V&VN HIV) are officially supporting Happi App.
Patient satisfaction and feedback
Design and functionality are scored between 4 and 5 on a 1-5 point scale. The net promotor score is 69. A patient panel of 30 patients advises the Happi App foundation regularly on current and future initiatives.
In summary
The Happi App is a valuable and easy to use addition to HIV-infected patients to give them more control over their health. It uses VBHC principles to optimize care for HIV.